You have a 24-year-old female with a history of juvenile rheumatoid arthritis, treated with hydroxychloroquine who sees you in clinic for a new consultation. She reports a history of dyspnea on exertion that has been slowly progressive over the previous six weeks. She is now short of breath with walking 40 steps on flat surface. She has no cough, sputum production, fevers, weight loss, or night sweats. She had worked on a farm and was exposed to mice, birds, ducks and rabbits starting eight weeks ago. There are mild inspiratory and expiratory wheezes on lung examination. PFTs from four years prior were normal but now demonstrate a very severe obstructive ventilatory defect, no significant response to bronchodilators, and air trapping and hyperinflation (TLC-133% and RV-326%).
Expiratory (top figure) and Inspiratory (bottom figure) cuts from Chest CT are shown below:
What is the most likely diagnosis?
Asthma
Hypersensitivity pneumonitis
Constrictive bronchiolitis
Allergic bronchopulmonary aspergillosis
Chronic bronchitis

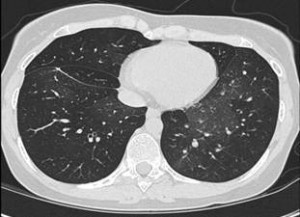
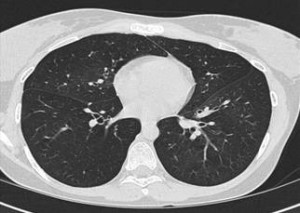
I think it is Constrictive bronchiolitis.
Although more common in Rheumatoid arthritis then Juvenile RA, it is still reported in the literature.
The combination of obstructive pattern on PFT with no bronchodilator effect associated with air trapping in a mosaic pattern in the expiratory CT cuts more then the inspiratory cuts is almost pathognomonic for this diagnosis.
What I am not sure about is whether or not there is a connection between Hydroxychloroquine and Constrictive bronchiolitis.
these are my resources:
– https://www-uptodate-com.sladenlibrary.hfhs.org/contents/bronchiolitis-in-adults?source=machineLearning&search=Constrictive+bronchiolitis&selectedTitle=1%7E150§ionRank=1&anchor=H48749157#H48749157
– http://www.ncbi.nlm.nih.gov/pubmed/16362444
– http://www.ncbi.nlm.nih.gov/pubmed/1578465
Constrictive bronchiolitis.
-lack of response to bronchodilator and air trapping thought not unique to obliterating bronchiolitis is characteristic
– thought positive with exposure the lack of ggo and nodular opacities (though OB can have it) argues against HP. Lack of bronchiectasis argues against ABPA
– some autoimmune in the background
– she has no coughing and sputum production