You have a 70 yo woman with COPD and HTN that was admitted to your ICU service 5 days ago in acute respiratory failure with sepsis due to CAP. She remains intubated and mechanically ventilated. She received early goal directed therapy and needed vasopressor support for the first 3 days of her ICU stay, but has now been weaned off vasopressors. She is on the PAD protocol and is awake, alert, not agitated, and following commands.
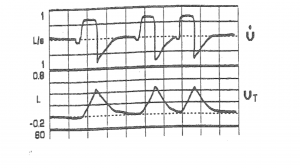
She remains hemodynamically stable and afebrile. She is on Volume assist-control with TV 6mL/kg IBW, RR 12, FiO2 40% and PEEP 5 cmH2O. O2 saturation is 92% and her pCO2 is normal (42mmHg). Ppk is 25 cmH2O Ppl 20 cmH2O. Her flow and volume tracing is below.
She undergoes weaning parameters which are acceptable, and starts a spontaneous breathing trial with PSV 7. After 10 minutes, she becomes agitated, hypertensive, tachycardic, and tachypneic with a respiratory rate of 32/min and O2 sat 85%. You place her back on full support with previous ventilator settings and see a Ppk 35 cmH2O and Ppl 30 cmH2O.
What does the rise in her airway pressures imply?
Which of the following would confirm the likely reason for her failure on the spontaneous breathing trial?
A) NIF (negative inspiratory force)
B) Troponin
C) Cuff leak test
D) Serum BNP level